Spondylolisthesis
(From the December 2003 The “G”Note)
Spondylolisthesis and spondylolysis are common findings in the chiropractic office. Some are symptomatic while many are incidental findings observed on physical examination and x-ray. This is a review on spondylolisthesis and spondylolysis and their chiropractic management using the Gonstead System.
Terminology
Spondylolisthesis: it’s Latin roots are the words spondylos = vertebra and olisthesis = slippage. (4,23) It is a defect in the pars interarticularis or degenerative apophyseal joint changes that is associated with anterior translation or slippage of the involved vertebral in relation to the subadjacent vertebra. (16,20)
Spondylolysis: lysis = dissolution, setting free, releasing, or loosening. (21) Spondylolysis may be unilateral or bilateral.
Incidence
The incidence range from 5% and upwards. (2,23). In the Caucasian population, the incidence is thought to be 5-7%. (3) The highest incidence of neural arch defects is in the Inuit where it is 40%. (23) Athletes appear to have a high incidence. (9,23) Within a family the incidence is five times greater than in near relatives (21).
Spondylolisthesis appears to be acquired after infancy as no cases of congenital isthmic defects have been found in the fetus. (2,10) Its appearance is first noted at ages 5-7 years with peak incidence around 10 years of age. (3,5) Boys are twice as likely as girls to have spondylolisthesis. (7,9) Degenerative spondylolisthesis is most commonly found over the age of 65 years, and L4 is the most common level of involvement. (11) Unlike pars defect-caused spondylolisthesis, the degenerative form is more common in women. (11,24) Disability due to spondylolisthesis does not appear to be greater than those with “non-specific” lower back pain. (14)
Spondylolisthesis is thought to be more common among young athletes than in the general population. Johnson states that 25%-39% of sports-related lower back pain may be associated with pars injuries. (9)This begs the question on the propriety of young children with immature skeletal systems engaging in high impact sports.
The most frequent site of pars defect spondylolisthesis is L5 where 70% to 90% are found. (4,23) The next most common site is 4L where 25% are found. (4,23). L1 to L3 and C5 to C7 are the location of 2% to 3% each. (23) In the chiropractic office, isthmic spondylolisthesis is typically seen at L5 and degenerative spondylolisthesis at L4/L5. At times, one finds both a degenerative L4 and isthmic L5 spondylolistheses in the elderly patient.
Types
There are various types of spondylolistheses. The primary types of interest to us are the isthmic and degenerative with pars interarticularis defect.
- Isthmic: the isthmic form may be a result of acute, stress, or fatigue fracture of the pars interarticularis (spondylolysis) or elongation of the intact pars.
- Degenerative form is usually associated with and secondary to spondylosis and posterior facet joint arthrosis without a true pars defect.
- Congenital or dysplastic form is due to developmental deficiency of the pars and is rare.
- Traumatic form is due to acute fracture.
- Pathological form is due to bone diseases, such as metastatic disease or TB that results in structural destructive changes.
- Iatrogenic: Some forms of spinal surgical procedures may cause a predisposition to spondylolisthesis.
Some use etiology and classify spondylolisthesis as acquired or developmental. (1)
Pseudospondylolisthesis are seen periodically. There are three types: 1) Abnormally long isthmus; 2) Predominately sagittally oriented facets with increased lumbosacral angle that can result in forward slip of L5; or 3) Apophyseal joints that are flatter or more sagittal than those above and below, there may be gradual degenerative changes or abnormal articular surface positions, and usually occurs at L4. (19)
In this article, we will be focusing on the L5 spondylolisthesis with spondylolysis due to pars defect as that is the most common form that we see in our offices.
Pars Interarticularis Defect
The pars interarticularis is the region between the superior and inferior articular processes. It is thought that the upright posture lends extra stress to the pars. (18,23) Flexion and extension put shear stress on this region. (9) Undue stress to this area, particularly if there is weakness or malformation, may lead to fracture or elongation of the pars. (18)
When a pars defect is present, the defect is usually filled with fibrocartilage whose coarse bands are anchored on opposing surfaces. When the gap is narrow, the opposing ends may be smooth, blunt, and eburnated with hyaline cartilage present in some cases. Larger gaps tend to have more fibrous tissue filling the defect. In a histological study of the tissues in the pars defect, a synovial-lined pseudoarthrodial cavity in the defect of spondylolysis in many of the samples, and the cavity often communicates with the facet joint immediately superior to it. (17)
Spondylolysis may be unilateral or bilateral. If unilateral, stress may be sufficient for the intact side to separate. (9) In Beutler’s study, some of the unilateral lesions healed. (2)
Is a Spondylolisthesis Stable?
In many cases, a spondylolisthesis is stable and does not progress. In a study that began in 1955 and ended in 1999, 30 individuals were studied with pars defects were studied. Of the 8 with unilateral pars defects, 3 had pars healing and no slippage was noted in the 8. Of the 22 with bilateral defects and spondylolisthesis, the average initial slip was 11%. In 1999, the average slip was 18%. Slippage was noted to decrease with age. (2) Floman’s study of 18 individuals with isthmic spondylolisthesis and severe lower back pain found 9% to 30% slip progression after the third decade of life which was thought to be due to disc degeneration at the spondylotic level. (6) Further slippage may occur in adults due to degeneration and trauma. In the immature spine, it may be associated with, in part, slippage of the osseoous and cartilagenous sacral base endplate. This may lead to the re-modeling changes to the sacral endplate characteristic of long term spondylolisthesis. (8)
Another aspect of the slippage is slippage of the immature vertebral endplate, i.e., between the osseous and still-cartilagenous endplates. (8)
Evaluation
There are some characteristic or classical findings. In the visual and static palpation, one may find the “spondylolisthotic shelf.” As one palpates along the spinous processes, one feels and may see a “step” or “shelf” formed by the spinous process. It is not uncommon, on motion palpation, to find unusual hypermobile motion at the spondylolisthotic segment. There may be a loss of the normal lumbar curve that is accompanied by trunk shortening, loss of the waistline,anterior and flank creases in the abdominal wall, and widening appearance of the iliac crests and flattening of the buttocks which gives the pelvis a heart-shaped appearance. (24) Some develop a waddle-type gait due to tight hamstrings, lumbar lordosis, posterior pelvic tilt, and a more vertically oriented sacrum. ((13) These may be the only physical findings present if subluxation, pathological process, and/or neurological disorders are not present.
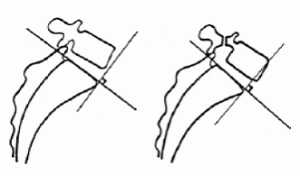
Meyerding developed a grading system for the degree of slippage. The system is based upon the amount of anterior slip found on the lateral x-ray. The sacral base is divided into four equal parts. The grading is the position of the posteriormost aspect of the vertebral body in relation to the sacral base. A Meyerding grade 1 indicates slippage of less that 25% (posteriormost 25% of the sacral base) over the sacral base. A grade 4 indicates the position of the posteriormost aspect of the vertebral is over the anteriormost 25% of the sacral base. (13,21,24) Although not a part of the original Meyerding grading system, many add a grade 5 for a vertebral body that completely anterior of the sacrum (21), and even a grade 6 for further anterior slippage well beyond the anterior margin of the anterior aspect of the sacrum. Another, more accurate measure, is Taillard’s measurement. On the lateral film, the A-P length of the L5 body is measured. The distance from the sacral posterior body to the L5 posterior body margin is measured. The percentage of slip is calculated: % of slip = (L5 body divided by slip distance) multiplied by 100. (13,24) There are a couple of methods of measuring the slip angle or sagittal rotation. One is the angle formed by the inferior L5 endplate and the sacral base endplate. (13) The other is the angle formed by the superior L5 endplate and a line perpendicular to a line along the posterior margin of S1 and S2. (24)
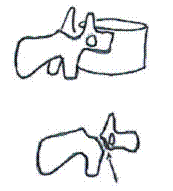
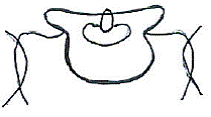
Other radiographic signs may also indicate the presence of a spondylolisthesis. The definitive view for pars defects is the oblique view. There are situations where the pars defect may not be visible on the oblique view due to the angle of the defect, this is especially problematic if there is spondylolysis without slippage. (15) In the lumbar spine, the pars (neck), transverse process (nose), pedicle (eye), inferior facet (front leg), and superior facet (ear) shadows create the image of a “Scotty dog.” A break in the “neck” indicates a pars defect and is called the “Scotty dog sign.” On the AP view of the lumbosacral region, superimposition of the displaced L5 body over the sacral base may produce increased opacity of the superior portion of the sacral base and create the Inverted “Napoleon’s Hat” Sign. is indicative of a L5 spondylolisthesis (12,19,23,24) If in the inferior aspect, the “Bowline of Brailford” sign may be present. (12,19,23) Another simple line drawing is Ullman’s line – a line drawn from a point at the anteriormost point of the sacral base that is perpendicular to a line parallel to the sacral endplate. If the L5 vertebral body bisects the line, a spondylolisthesis may be the cause. (12,19,23)
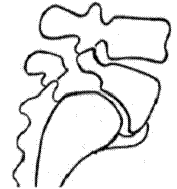
Classical, long-standing features on the lateral x-ray of a lumbosacral spondylolisthesis are a markedly trapezoid-shaped L5 vertebral body (taller anterior than posterior), calcified buttressing of the anterior ligament, and doming of the superior surface of the sacral base. (1,19,23)
Chiropractic Correction
Just because a spondylolisthesis is present, whether accompanied by symptoms in that area or not, does not justify adjustments to that segmental level unless it is a subluxation. Even if low back complaints are present with a L5 spondylo’, the actual subluxation may be elsewhere. Not uncommonly, it is found in the mid- to upper lumbar spine or the lower thoracic region. I took car of a father and son, both of whom had low back pain and L5 spondylolistheses. One required sacral adjustments while the other, T12 adjustments. A great truism is Dr. Gonstead’s statement, “Find the subluxation. Accept it where you find it.”
In the Gonstead System, if the level of the spondylolisthesis is the subluxation, we adjust the subadjacent vertebra. If L5, the sacrum is adjusted as a base posterior. The S1 tubercle is the usual contact. If the S1 tubercle is difficult to discern, one can contact S2 tubercle. Unlike the “rolling” I-S line-of-correction of the sacral base posterior, the LOC has a slight S-I component to fit the sacrum under the spondylo’. It is not uncommon for the subluxation level to change as correction is effected. In a common scenario of a L5 spondylolisthesis that requires sacral adjustments, the sacral base is adjusted P-A. If he patient improves but plateaus, it is not unusual for the subluxation to shift to the L2 to L4 area or higher and further correction requires recognizing the change and adjusting accordingly.
As in all corrections of subluxations, finding the right adjustment and table is critical. When an L5 subluxation and spondylolisthesis is found, it is common to adjust the sacrum as a side posture, pisiform push move. There are many cases where the Hylo table (prone table) or knee chest table is the most effective.
If acute spondylolysis is suspected but not viewed on plain x-ray and, in particular, if there is skeletal immaturity, some advise bone scans or SPECT studies. If the risk of further slippage is deemed high, a discussion of the risk of engaging high-risk activities, such as football or gymnastics would be advisable.
The medical treatment includes avoidance of high-risk activities and observation, decompression, fusion, and fusion cages.
Rarely does one see significant posterior body margins re-alignment during correction, despite symptoms abating and physical findings improving. It is more common to see improvement in the angulation of the spondylotic vertebra to the subadjacent vertebra. Some feel that a common pain generator may be the L4/L5 zygapophyseal joints as a result of extreme extension as a compensation to the L5 spondylo’, and adjustments to the sacral base may reduce the stress on those joints. Maintaining optimal spinal function is very important to patients with spondylolisthesis, symptomatic or not.
Fig.1 Meyerding Grades #1 & #3
Fig.6 Lumbosacral changes to L5/sacrum
References
1. Antoniades SB. Hammerberg KW, DeWald RL. Sagittal Plane Configuration of the Sacrum in Spondylolisthesis. Spine 2000; 25(9):1085-1091.
2. Beutler WJ, et al. The Natural History of Spondylolysis and Spondylolisthesis: 45-Year Follow-up Evaluation. Spine 15 May 2003; 28(10):1027-1035.
3. Bull P, et al. The Effects of Spondylolisthesis on the Lumbar Spine: A Cross-Sectional Radiological Survey. Chiropr J Aust Mar 2000; 30(1):5-12.
4. Calliet R. Low Back Pain Syndrome. Philadelphia: F.A. Davis Co. 1981. p.187.
5. Farfan HF. Mechanical Disorders of the Low Back. Philadelphia: Lea & Ferbiger. 1973. pp.162-163.
6. Floman Y. Progression of Lumbosacral Isthmic Spondylolisthesis in Adults. Spine 1 Feb 2000; 25(3):342-347.
7. Fredrickson BE, et al. The Natural History of Spondylolysis and Spondylolisthesis. J Bone Joint Surg June 1984; 66-A(5):699-707.
8. Inoue H, Ohmori K, Miyasaka K. Radiographic Classification of L5 Isthmic Spondylolisthesis As Adolescent or Adult Vertebral Slip. Spine 15 Apr 2002; 27(8):831-838.
9. Johnson RJ. Low-Back Pain in Sports. Physician and Sportsmed Apr 1993; 21(4):53-59.
10. Leach RA. The Chiropractic Theories: A Synopsis of Scientific Research (2d ed). Baltimore: Williams & Wilkins. 1986. pp.44-45.
11. Love TW, Fagan AB, Fraser RD. Degenerative Spondylolisthesis. J Bone Joint Surg July 1999; 81-B(4):670-674.
12. MacRae JE. Roentgenometrics in Chiropractic. CMCC lecture notes.
13. Massari MA. Spondylolisthesis Evaluation, Management and Long-Term Prognosis. J Am Chirop Assoc Sept 1997; 34(():41-46.
14. Möller H, Sundin A, Hedlund R. Symptoms, Signs, and Functional Disability in Adult Spondylolisthesis. Spine 15 Mar 2000; 25(6):683-689.
15. Saifuddin A, et al. Orientation of Lumbar Pars Defects. J of Bone Joint Surg Mar 1998; 80-B(2):208-211.
16. Shafer RC. Clinical Biomechanics: Musculoskeletal Actions and Reactions. Baltimore: Williams & Wilkins. 1983.
17. Shipley JA, Beukes CA. The Nature of the Spondylolytic Defect. J Bone Joint Surg July 1998; 80-B(4):662-664.
18. Taillard WF. Etiology of Spondylolisthesis. Clin Orthop Rel Res. June 1976; 117:30-39
19. West HG. LACC Chiropractic Orthopedic Notes. 1985-6.
20. White AA, Panjabi MM. Clinical Biomechanics of the Spine. Philadelphia: J.B. Lippincott Co. 1978.
21. Wiltse LL, Newman PH, MacNab I. Classification of Spondylolysis and Spondylisthesis. Clin Orthop Rel Res. June 1976; 117:23-29.
22. Wright IP. Who Was Meyerding? Spine 1 Apr 2003; Spine 28(7):733-735.
23. Yochum TR. Three-In-One seminar notes. Feb 1986.
24. Yu C, Garfin R. Recognizing and Managing Lumbar Spondylolisthesis. J Musculoskeletal Med Nov 1994; 11(11):55-64.