Lateral Lumbar Spine: Line Marking
(From December 2004 The ‘G” Note )
The Gonstead x-ray analysis of the lateral cervical spine view includes a series of endplate lines drawn from C2 to C7. These lines are used to assess the relative rotation angles in +/–X (flexion and extension) of each vertebra compared to the next one below it — i.e., on the lateral film, there is an angle formed by a line drawn through the inferior vertebral end-plate of the superior segment to that of the inferior endplate of the subadjacent vertebra. These lines are then used to infer which vertebra may be misaligned. This same level of scrutiny can be applied to the lumbar spine; however, it is not traditionally included nor taught in the Gonstead line marking system.
The Gonstead lateral cervical line marking theory states that each of the endplate lines should equally converge at some point several inches posterior to the cervical spine when the cervical spine shows a smooth and normal lordotic configuration. When one line crosses the subadjacent line prior to the convergence point of the lines of nearby levels, this suggests an extension malposition of the vertebra. This hyperextension misalignment suggests subluxation, the confirmation of which must be made in correlation with the full assessment of the patient.
The normal relative rotation angles (X or flexion-extension angles) between segments in the cervical spine have been reasonably well investigated. Troyanovich, in his book, Structural Rehabilitation of the Spine and Posture, lists tables of normal ranges of relative rotation angles between each vertebrae from C2/C3 through C6/C7. Each level is shown to rotate to a relatively equal degree to the one below it in the –X direction (extension): the relative rotation angles were –4.0 to –6.5 degrees per level from C3/C4 through C6/C7. At C2/C3, the relative rotation angles are slightly higher, normally from –5.0° to –8.0°. The support given for these angles is relatively sound as based upon the literature reviewed by Troyanovich in preparation of this table, and for the purposes of this discussion, will be assumed to be accurate. Readers are directed to that text for further investigation of the specific data used to compute these normal ranges. These normal values for the cervical spine support the Gonstead method of lateral cervical line marking as described above.
Troyanovich also summarized values that have been reported on the lumbar spine. The clinical observations by this author concur with those listed as ranges of normal values for relative rotation between vertebrae in the lumbar spine. This author has long noted a tendency for the lumbar spine to show relative rotation angles that are somewhat more acute in the lower lumbar spine. The degree of inter-segmental extension will incrementally diminish at each progressively higher level of the lumbar spine. According to Troyanovich’s summary, the relative rotation angle at L5/S1 typically ranges between –21 to –25 degrees, significantly more than what is seen in the cervical spine. Between L4/L5, the range is –15° to –20°; L3/L4 is –11° to –13°; L2/L3 is –6° to –10°; and L1/L2 is –2° to –4°. There is very little extension of L1 upon L2 compared to the extension of L5 upon S1 in the normal lordotic configuration of the lumbar spine.
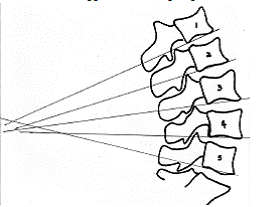
When endplate lines are drawn consecutively, using the inferior endplate of the vertebral body from L5 through L1, you should see a gradually reduced convergence of the lines at the posterior. L4 line should cross the L5 line slightly before the L3 line, and L3 crosses the L5’s endplate line slightly before L2, and so on. Superiorward, the intersection of the lines upon each other becomes more posterior incrementally, smoothly and equally at each higher level of the lumbar spine, such that, the upper lumbar plane lines may not cross on the film but only converge slightly. [see figure 1]
Fig. 1: In ascending order, all lines converge posterior to the subadjacent vertebral line
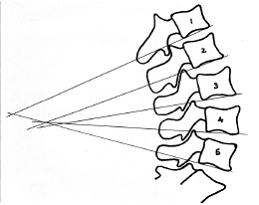
When you see a vertebra such as L3 crossing the line of L4 before the L4 line crosses the line of L5, you are likely observing an abnormality reflective of intersegmental biomechanical fault. [see figure 2]
Fig. 2: The postero-inferior L3 line converges before the L4 line.
Likewise, when you see a level that is converging less than it should, this is potentially a compensation or an injury. These misalignments are supportive but not conclusive of subluxation or compensation. These x-ray findings must be corroborated with other patients findings to determine their true significance.
The purpose of this article is to point out that one should evaluate the lateral lumbar spine intersegmentally in a similar fashion to what one does in the cervical spine, rather than merely “eyeballing” it. There is no reason why the Gonstead system should not include a more specific line assessment on the lateral lumbar spine view in a like manner to the cervical spine.
One hopes that this presentation will result in further discusssion, such that it can be incorporated as part of a consistently presented package of x-ray line marking.
There are other useful lateral lumbar spine marking procedures that could and should be added to the basic work of the Gonstead technique radiographic analysis. These include the measurement of retrolisthesis or anterolisthesis, the overall lumbar curve, Cobb’s angle, sacral base angle, and other useful determinates of biomechanical faults that should be part of the basic x-ray assessment. If one is going to take the time, energy, and potential risk of radiologic exposure, the full advantages should be taken of radiographic analysis.
It is far too often that x-rays are taken and assessed for a single visit and not referred to periodically during the course of care as required to ensure accuracy of the adjustments. Those that do not pay close attention to x-ray assessment and its application to ongoing care are often missing clues to effectively care for their patients while simultaneously limiting learning experiences that build a practitioner into an expert.